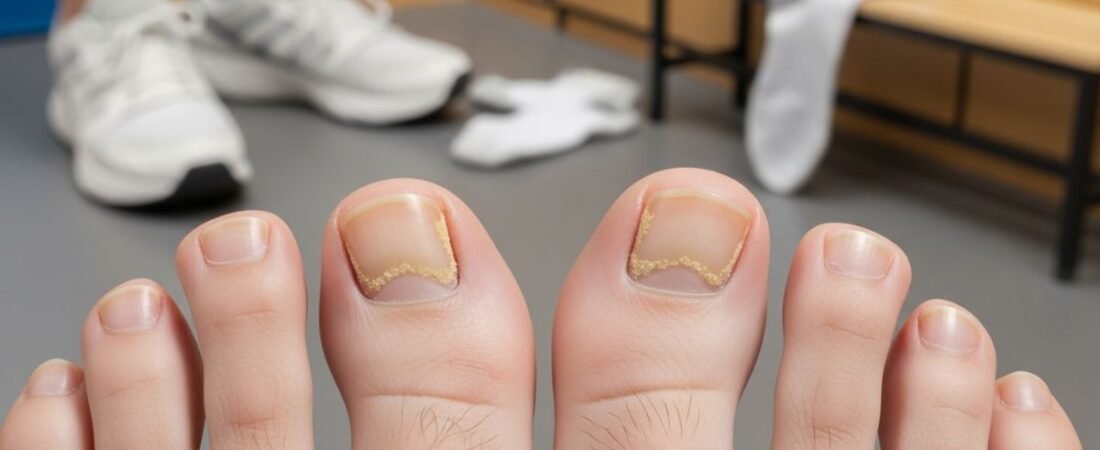
Toenail fungus is often dismissed as a minor or cosmetic issue. In reality, it is a progressive fungal infection that tends to worsen over time if left unaddressed. While many people are exposed to fungal organisms, not everyone develops a persistent nail infection. The difference lies largely in risk factors.
Understanding the risk factors for toenail fungus is essential for early detection and prevention. Certain health conditions, lifestyle habits, and environmental exposures significantly increase susceptibility, especially in adults and older populations. Recognizing these factors early can reduce complications and long-term nail damage.
This article examines the most important toenail fungus risk factors you should not ignore, with a focus on evidence-based health connections rather than treatment promotion.
What Is Toenail Fungus?
Toenail fungus, medically referred to as onychomycosis, is a fungal infection affecting the nail plate, nail bed, or surrounding tissue. It is most commonly caused by dermatophyte fungi, although yeasts and molds may also be involved.
The infection develops slowly, often beginning with subtle discoloration or texture changes. Over time, the nail may thicken, become brittle, or separate from the nail bed.
Why Identifying Risk Factors Matters
Fungal spores are widespread in the environment. Exposure alone does not guarantee infection. Risk factors determine whether fungi can successfully colonize the nail and persist.
Identifying these factors helps individuals:
- Recognize early warning signs
- Reduce exposure and recurrence
- Understand why infections may persist
- Take preventive action before progression
Major Toenail Fungus Risk Factors
1. Diabetes and Blood Sugar Imbalance
One of the most significant and well-documented risk factors for toenail fungus is diabetes.
Chronically elevated blood sugar can impair immune response, reduce circulation to the feet, and slow nail growth. These changes create an environment where fungal organisms can thrive.
People with insulin resistance or type 2 diabetes may also experience nerve damage, reducing awareness of early nail changes. As a result, infections are often detected later.
Managing blood sugar levels plays a critical role in prevention. Educational resources explaining how diabetes affects infection risk can be helpful, such as this detailed guide on blood sugar control and systemic health:
👉 Why People With Diabetes Are More Prone to Nail Infections
This type of information-focused content supports prevention rather than treatment claims.
2. Poor Circulation in the Lower Extremities
Reduced blood flow to the feet limits oxygen and immune cell delivery to the nail bed. This weakens the body’s natural defense against fungal organisms.
Circulatory issues are more common in:
- Older adults
- Individuals with diabetes
- People with cardiovascular conditions
- Sedentary individuals
When circulation is compromised, nail infections become harder to clear naturally.
3. Nail Trauma or Repeated Pressure
Even minor nail trauma can increase the risk of fungal infection.
Examples include:
- Tight or ill-fitting shoes
- Repeated pressure from athletic activity
- Nail cracking or splitting
- Aggressive trimming or pedicures
Trauma creates micro-openings in the nail structure, allowing fungi to enter and establish infection.
4. Moist Environments and Footwear Habits
Fungi thrive in warm, moist conditions. Prolonged moisture exposure significantly raises infection risk.
Common contributors include:
- Sweaty feet
- Non-breathable shoes
- Wearing damp socks
- Shared locker rooms or showers
Toenails trapped in moist environments for long periods become especially vulnerable.
5. Age-Related Changes
Age is an independent risk factor for toenail fungus.
As people age:
- Nail growth slows
- Nails become thicker and more brittle
- Circulation may decline
- Immune response weakens
These changes make fungal infections more likely and slower to resolve.
6. Compromised Immune System
Any condition or medication that weakens immune function increases fungal susceptibility.
This includes:
- Autoimmune disorders
- Long-term corticosteroid use
- Certain cancer treatments
- Chronic stress
When immune surveillance is reduced, fungal organisms face less resistance.
7. Skin Conditions Affecting the Feet
Skin conditions such as athlete’s foot (tinea pedis) often coexist with toenail fungus.
Cracked or inflamed skin around the toes provides a direct pathway for fungi to spread into the nail bed. Untreated skin infections frequently precede nail involvement.
Early Signs People Often Miss
Risk factors increase susceptibility, but early symptoms are often subtle.
Common early indicators include:
- Slight yellow or white nail discoloration
- Mild nail thickening
- Brittle or uneven nail edges
- Slow changes in nail shape
- Loss of natural nail shine
Understanding what toenail fungus looks like in its early stages can help individuals act before the infection advances. Visual education resources can support early awareness and prevention.
Why Toenail Fungus Is More Than a Cosmetic Issue
While toenail fungus may begin as a cosmetic concern, progression can lead to functional and health-related complications, especially in high-risk individuals.
Potential issues include:
- Nail pain or pressure discomfort
- Difficulty trimming nails
- Secondary bacterial infections
- Increased foot injury risk
- Complications in people with diabetes
For this reason, early identification of risk factors is essential.
Prevention Strategies Based on Risk Reduction
Addressing risk factors does not guarantee prevention, but it significantly lowers susceptibility.
Evidence-based prevention strategies include:
- Maintaining healthy blood sugar levels
- Wearing breathable footwear
- Keeping feet clean and dry
- Inspecting nails regularly
- Avoiding aggressive nail care
- Treating athlete’s foot promptly
Consistency is key, particularly for individuals with multiple risk factors.
When to Seek Professional Evaluation
Medical advice should be considered if:
- Nail discoloration worsens
- Nail thickening causes discomfort
- Nails separate from the nail bed
- Redness or swelling appears
- Infection does not improve over time
Early evaluation allows safer and more effective management, especially for people with underlying health conditions.
Conclusion
Toenail fungus rarely develops without contributing factors. Conditions such as diabetes, poor circulation, nail trauma, aging, and immune compromise significantly increase susceptibility. Recognizing these risk factors early allows individuals to monitor nail health more closely and reduce the likelihood of progression.
Toenail fungus is not merely cosmetic. For at-risk populations, it is a health signal that should not be ignored.